Prescribing calls
Sam and Vani explore the most common requests for after hours prescribing and how to safely and quickly approach prescribing of insulin, warfarin, analgesia, antiemetics, and sleeping tablets.
Insulin
- Generally treat any blood glucose of 20 or above.
- Target range:
- Inpatient: 7 – 14 mmol/L
- Outpatient: 4 – 10 mmol/L
- Achieving target 60% of the time is quite good!
- Neglecting high BSLs leads to irritating symptoms, opportunistic infections and delayed recovery.
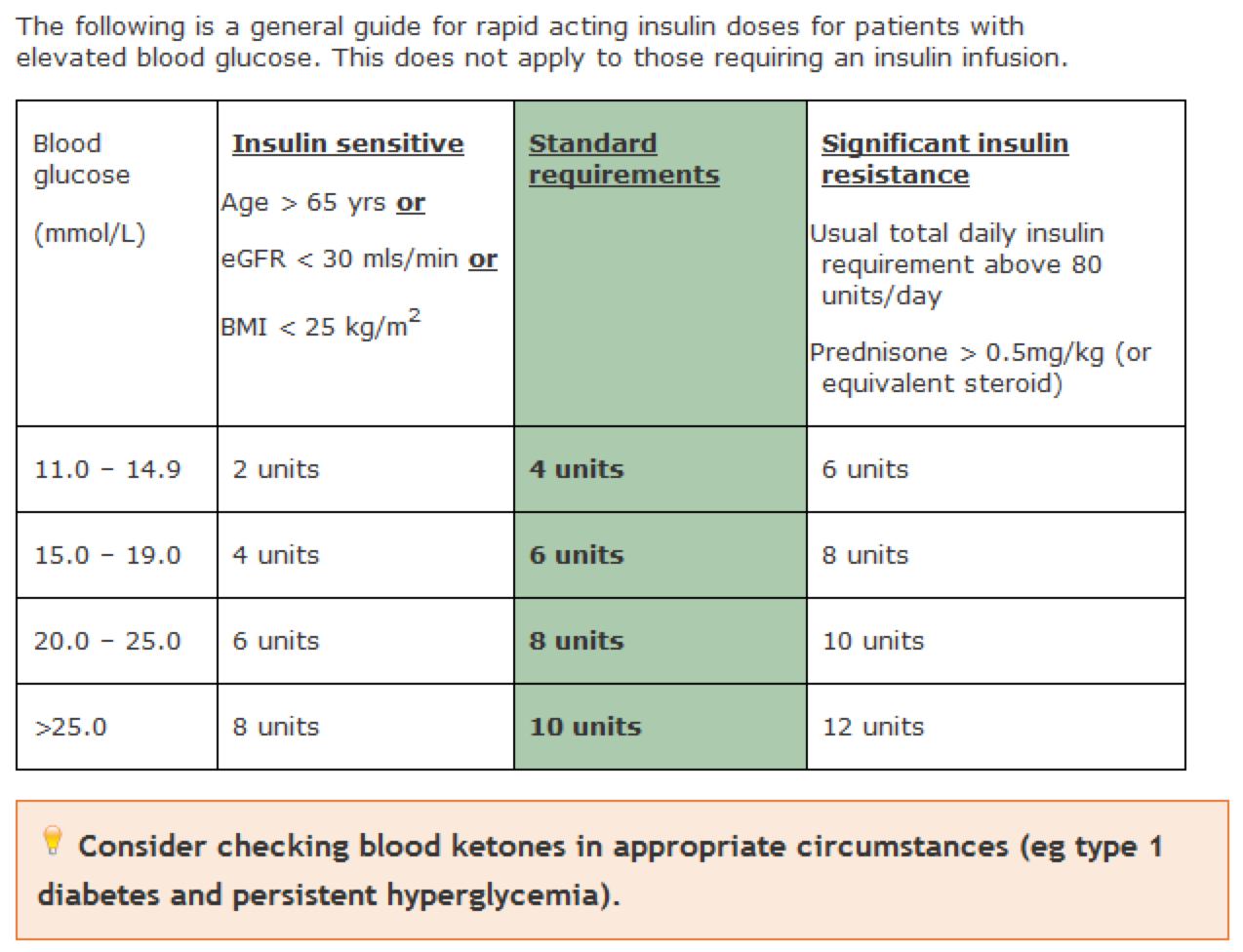
- Correct BSLs with a rapid acting insulin (Novorapid)
- Correction doses should be given at meals and no more frequently than 4 hourly.
- If correction doses of insulin are required, consider increasing the person’s usual insulin / treatment.
- Don’t recheck BSLs too early. Wait until the next scheduled check, unless there is concern of hypoglycaemia.
- Don’t use ActRapid – it works slowly subcut so should only be used IV.
- Diabetes in pregnancy requires frequent adjustment and tighter control – consult a senior.
- Don’t withhold long acting insulin (Lantus and insulin degludec) if NBM, even if on a GIK.
Antiemetics
- Cyclizine (NZF)
- Antihistimine
- Classic, old-school, and effective
- Great for non-iatrogenic nausea and vomiting
- Can give euphoria IV, so avoid in young patients specifically requesting it and in the elderly
- 25 – 50 mg PO/IV TDS PRN
- Ondansetron (NZF)
- Serotonin antagonist
- Newer, but not necessarily better antiemetic
- Primarily indicated for PONV and chemotherapy-induced nausea
- Can be constipating
- Can reduce the effectiveness of tramadol, so avoid co-prescription
- 10 mg PO/IV TDS PRN
- Metoclopramide (NZF)
- Dopamine antagonist
- Gastric stimulant, avoid in suspected small bowl obstruction
- Avoid co-prescribing with droperidol and prochlorperizine
- Avoid in Parkinson’s disease
- Avoid in under 20 year olds due to risk of oculogyric crisis
- 10 mg PO/IV TDS PRN
- Domperidone (NZF)
- Somewhat interchangeable with metoclopramide, but no IV formulation
- Does not cross BBB, so preferred in Parkinson’s disease
- 10 mg PO TDS PRN
- Droperidol (NZF)
- Dopamine antagonist
- Usually prescribed by anaesthetics for PONV
- 0.625–1.25 mg IV Q6H PRN
- Scopoderm patch (NZF)
- Nonspecific antimuscarinic
- Usually prescribed by anaesthetics for PONV
- 1 patch Q72H
- Prochlorperazine (NZF)
- Oral: 20 mg initially then 10 mg after 2 hours; prevention 5–10 mg 2–3 times daily
- Rectal: 25 mg when required followed if necessary after 6 hours by an oral dose, as above
- Don’t confuse with chlorpromazine!
Analgesia
- Pain assessment
- Try to get some kind of assessment documented e.g. verbal pain score
- Pain ladder
- Simple analgesia e.g. paracetamol +/- NSAID
- “Weak” opioides e.g. tramadol or codeine
- Titrate up opiates e.g. morphine or oxycodone
- It may be necessary to “get on top” of the pain first with some IV boluses, then once the patient is comfortable, some low-dose long acting analgesia may be all that is required.
- If possible, please avoid opiates in young patients (e.g. <25 years) as there is a strong link between opiate exposure in the young and subsequent drug and alcohol dependance and abuse. First do no harm!
Sleeping tablets
- Very common request on evening and ward calls
- Balance benefit with risk
- Patients need sleep to recover from the illness, so don’t withhold unnecessarily
- However don’t contribute to an avoidable fall
- Zopiclone (NZF)
- 7.5 – 15 mg PO nocte
- Generally first line unless the patient already uses an alternative
- Quetiapine (NZF)
- Antipsychotic, not indicated for insomnia
- However patient who have tried it tend to swear by it
- Use as a sleeping tablet in low dose (e.g. 25 mg) is off-label, so generally avoid unless the patient already uses it.
- Benzodiazepines
- Temazepam (NZF) 10 – 20 mg PO nocte
- Generally avoid benzos unless you are experienced with their use, as they have many interactions and dependance is rapid.
